
Digestive discomfort in children is often minimized, misinterpreted, or attributed to temporary sensitivity. Yet, in some cases, recurring symptoms may point to a deeper underlying issue.
Lucas’ story illustrates how lactose intolerance in children can remain unrecognized for years, affecting not only digestive health but also growth, comfort, focus, and quality of life. His experience also highlights the importance of early diagnosis and appropriate nutritional management.
Lucas’ Story: A Parent’s Perspective
Early Symptoms in Infancy

“Ever since he was a baby, my little Lucas regularly spat up his feeds, was often restless, and suffered from colic. Doctors prescribed various anti-nausea and anti-diarrhea medications, but nothing seemed to truly solve the problem.
He was not gaining much weight, and we started to worry that he might be falling behind in his growth.”
In infancy, digestive symptoms are often difficult to interpret. Spitting up, irritability, and feeding-related discomfort can sometimes be considered common or temporary. However, when these symptoms persist or are associated with poor weight gain, closer investigation may be needed.
Years of Digestive Discomfort
“As he grew older, my child continued to suffer from recurring stomach aches, diarrhea, and discomfort for years. We consulted several doctors, but the symptoms were often attributed to food sensitivity or anxiety.”
Like many children with digestive complaints, Lucas’ symptoms did not immediately lead to a clear diagnosis. Recurrent abdominal pain, bloating, discomfort and diarrhea are common in pediatric consultations and can easily be confused with other conditions such as functional abdominal pain, food allergies or generalized digestive sensitivity.
The Turning Point: Diagnosis and Improvement
“Finally, after persistent testing, we received a diagnosis of lactose intolerance. By adapting both diet and treatment, my child’s health improved drastically. Lucas is now growing very well and developing normally. At school, he is calmer, less distracted and better able to concentrate.”
This turning point changed daily life not only at home, but also at school. What had seemed like isolated digestive issues turned out to be part of a broader pattern with direct consequences on physical comfort, emotional wellbeing and concentration.
Lucas’ case shows how early identification of lactose intolerance could prevent years of avoidable discomfort.
Why Lactose Intolerance in Children Can Be Missed
Symptoms Often Overlap with Other Conditions
Lactose intolerance in children is often under-recognized because its symptoms are not always specific. Pediatric digestive symptoms may overlap with:
● functional abdominal pain
● food allergies
● irritable bowel-type symptoms
● anxiety-related digestive complaints
● post-infectious digestive sensitivity
Because these symptoms are common and often nonspecific, lactose malabsorption may not be considered immediately.
Why Early Recognition Matters
When digestive symptoms become chronic, children may experience more than gastrointestinal discomfort. Repeated pain, bloating and diarrhea can affect:
● appetite
● nutritional intake
● school concentration
● sleep quality
● mood and social comfort
In some cases, delayed recognition may also affect normal growth and development.
Scientific Context: Lactose Intolerance in Pediatric Populations
Gastrointestinal complaints represent approximately 10–15% of pediatric consultations. Lactose malabsorption may contribute in a subset of cases. Within this broad group, lactose malabsorption may be a contributing factor in a subset of children.
Although lactose intolerance in children is relatively uncommon, it remains clinically important when present. If not properly identified and managed, it can interfere with gastrointestinal function, nutritional status and normal growth.
Lactose intolerance in children is therefore not only a question of digestive discomfort. In some cases, it has broader clinical implications that justify timely recognition and careful follow-up.
Pathophysiological Background
The Role of Lactose in Early Life
In infancy and early childhood, lactose is an important carbohydrate. It is naturally present in breast milk and in standard infant formulas and contributes to several key physiological functions, including:
● energy supply
● calcium absorption
● development of the intestinal microbiota
In fact, lactose may account for a substantial proportion of caloric intake in early life, making normal digestion particularly important during growth.
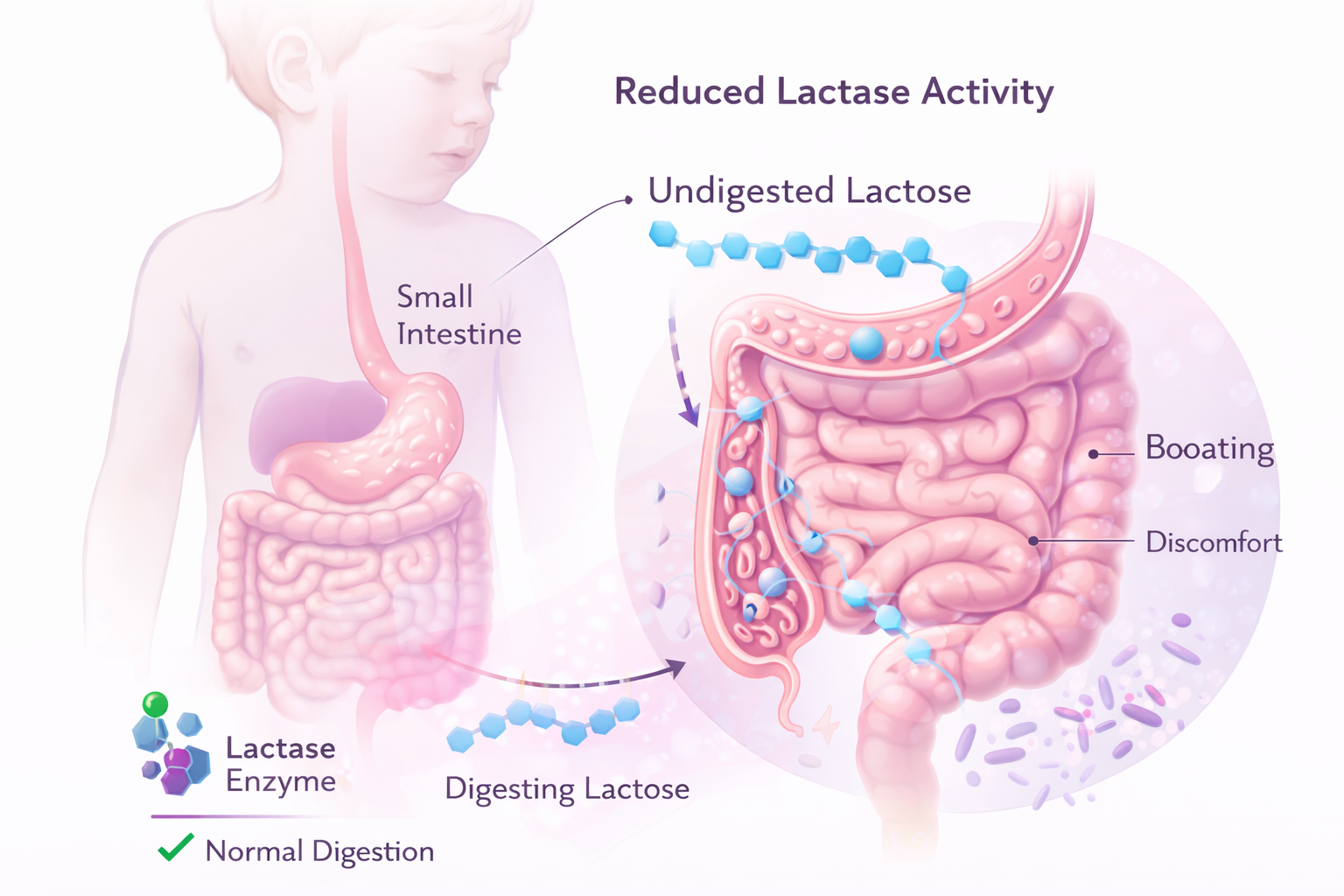
When Lactase Activity Is Reduced
Lactose intolerance in children occurs when lactase activity is reduced, leading to incomplete digestion of lactose in the small intestine.
This may happen in specific situations such as:
● congenital lactase deficiency, an extremely rare condition estimated at fewer than
1 in 60,000 births
● secondary lactose intolerance, which may occur after gastrointestinal infections or
intestinal mucosal injury
When lactose is not properly digested, it passes into the colon where it is fermented by bacteria, contributing to digestive symptoms.
Clinical Manifestations of lactose intolerance in Children
Digestive Symptoms
Undigested lactose in the colon may lead to symptoms such as:
● diarrhea
● abdominal distension
● bloating
● excessive gas
● stomach aches
● irritability
In younger children, symptoms may be more difficult to express verbally and may instead appear as restlessness, feeding discomfort or unexplained crying.
Potential Developmental Consequences
If symptoms persist and lactose intolerance remains unrecognized, some children may experience broader consequences, including:
● dehydration due to persistent diarrhea
● electrolyte imbalance
● impaired weight gain
● delayed growth
● reduced calcium absorption during a critical phase of bone development
Because childhood is a period of rapid physical and cognitive development, even relatively short periods of malabsorption may have measurable effects.
Clinical Evidence
Studies suggest that secondary lactose intolerance in children is relatively common after acute gastroenteritis in infants and young children. In such cases, transient lactase deficiency may persist for a period of time after the intestinal lining has been affected.
Clinical observations may include:
● increased stool acidity, often with a pH below 5.5
● presence of reducing substances in stool
● symptom improvement after lactose elimination
● resolution within 1 to 4 weeks in transient cases
By contrast, congenital lactase deficiency requires long-term or lifelong dietary management.
These distinctions are important because not all lactose intolerance follows the same clinical course. Proper diagnosis helps guide the right nutritional and therapeutic decisions.
Nutritional and Developmental Impact
Lactose intolerance in children should never be reduced to a simple dietary inconvenience. When persistent, it can affect essential aspects of development.
Potential consequences include:
● poor caloric intake due to digestive discomfort
● reduced tolerance to feeding
● impaired growth trajectory
● decreased calcium intake or absorption
● nutritional imbalance if dietary changes are poorly managed
For this reason, any dietary adaptation must be supervised carefully to ensure the child continues to receive adequate:
● calcium
● vitamin D
● total calories
● essential nutrients
Clinical Management
Dietary and Medical Adaptation
Management depends on the underlying cause of lactose intolerance in children.
In cases of secondary lactose intolerance, clinicians may consider:
● temporary lactose-free or low-lactose formulas
● adapted diet under supervision
● gradual reintroduction of lactose after intestinal recovery
In mild situations, breastfeeding may sometimes continue with medical guidance depending on the child’s tolerance and overall clinical context.
In congenital lactase deficiency, a strict long-term lactose-free nutritional approach is generally required.
Monitoring Growth and Nutritional Needs
Children diagnosed with lactose intolerance should be monitored to ensure that dietary restriction does not create nutritional deficiencies.
Clinical follow-up may include:
● growth monitoring
● symptom evolution
● dietary assessment
● calcium and vitamin D balance
The goal is not only to reduce digestive symptoms, but also to support normal development.
The Role of Early Diagnosis

Dietary and Medical Adaptation
Lactose intolerance in children should be distinguished from other conditions that may present similarly,
including:
● cow’s milk protein allergy
● functional gastrointestinal disorders
● infectious diarrhea
● nonspecific digestive sensitivity
Without appropriate differentiation, children may receive incomplete or inaccurate
management.
Diagnostic Approaches
Depending on the clinical situation, diagnostic approaches may include:
● stool analysis
● clinical response to lactose elimination
● evaluation of symptom timing after lactose intake
● genetic testing in rare congenital cases
Accurate diagnosis is essential not only for symptom relief, but also for long-term nutritional
management and reassurance for families.
Lactose intolerance in children FAQ
What are the symptoms of lactose intolerance in children?
Children with lactose intolerance may experience stomach pain, bloating, diarrhea, gas and digestive discomfort. In some cases, symptoms may also affect concentration, mood and daily comfort.
Can lactose intolerance affect a child’s growth?
Yes. If it is not recognized and properly managed, lactose intolerance may contribute to poor weight gain, digestive distress and nutritional imbalance during an important stage of growth.
Why is lactose intolerance in children often misdiagnosed?
Its symptoms can overlap with other common conditions such as food allergies, functional abdominal pain or general digestive sensitivity, which may delay proper diagnosis.

